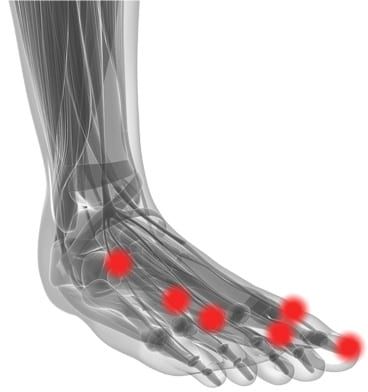
What Is a Neuroma? Aneuroma is a thickening of nerve tissue that may develop in various parts of the body. The most common neuroma in the foot is a Morton’s neuroma, which occurs at the base of the third and fourth toes. It is sometimes referred to as an intermetatarsal neuroma. “Intermetatarsal” describes its location—in the ball of the foot between the metatarsal bones (the bones extending from the toes to the midfoot). Neuromas may also occur in other locations in the foot. The thickening, or enlargement, of the nerve that defines a neuroma is the result of compression and irritation of the nerve. This compression creates swelling of the nerve, eventually leading to permanent nerve damage. Symptoms of a Morton’s Neuroma If you have a Morton’s neuroma, you will probably have one or more of these symptoms where the nerve damage in occurring:
- Tingling, burning, or numbness
- Pain
- A feeling that something is inside the ball of the foot, or that there’s a rise in the shoe or a sock is bunched up The progression of a Morton’s neuroma often follows this pattern:
- The symptoms begin gradually. At first they occur only occasionally, when wearing narrow-toed shoes or performing certain aggravating activities.
- The symptoms may go away temporarily by massaging the foot or by avoiding aggravating shoes or activities.
- Over time the symptoms progressively worsen and may persist for several days or weeks.
- The symptoms become more intense as the neuroma enlarges and the temporary changes in the nerve become permanent.
What Causes a Neuroma?
Anything that causes compression or irritation of the nerve can lead to the development of a neuroma. One of the most common offenders is wearing shoes that have a tapered toe box, or high-heeled shoes that cause the toes to be forced into the toe box. People with certain foot deformities—bunions, hammertoes, flatfeet, or more flexible feet—are at higher risk for developing a neuroma. Other potential causes are activities that involve repetitive irritation to the ball of the foot, such as running or racquet sports. An injury or other type of trauma to the area may also lead to a neuroma. Diagnosis To arrive at a diagnosis, the podiatric foot and ankle surgeon will obtain a thorough history of your symptoms and examine your foot. During the physical examination, the doctor attempts to reproduce your symptoms by manipulating your foot. Other tests may be performed. The best time to see your podiatric surgeon is early in the development of symptoms. Early diagnosis of a Morton’s neuroma greatly lessens the need for more invasive treatments and may avoid surgery. Treatment In developing a treatment plan, your podiatric surgeon will first determine how long you’ve had the neuroma and evaluate its stage of development. Treatment approaches vary according to the severity of the problem. Lateral plantar nerve Medial plantar nerve Neuroma Common digital nerves For mild to moderate cases of neuroma, treatment options include:
- Padding. Padding techniques provide support for the metatarsal arch, thereby lessening the pressure on the nerve and decreasing the compression when walking. • Icing. Placing an icepack on the affected area helps reduce swelling.
- Orthotic devices. Custom orthotic devices provided by your podiatric surgeon provide the support needed to reduce pressure and compression on the nerve.
- Activity modifications. Activities that put repetitive pressure on the neuroma should be avoided until the condition improves.
- Changes in shoewear. It’s important to wear shoes with a wide toe box and avoid narrow-toed shoes or shoes with high heels.
- Medications. Nonsteroidal antiinflammatory drugs (NSAIDs), such as ibuprofen, help reduce the pain and inflammation.
- Injection therapy. If there is no significant improvement after initial treatment, injection therapy may be tried.
When Is Surgery Needed?
Surgery may be considered in patients who have not received adequate relief from other treatments. Generally, there are two surgical approaches to treating a neuroma— the affected nerve is either removed or released. Your podiatric surgeon will determine which approach is best for your condition. The length of the recovery period will vary, depending on the procedure or procedures performed. Regardless of whether you’ve undergone surgical or nonsurgical treatment, your podiatric surgeon will recommend long-term measures to help keep your symptoms from returning. These include appropriate footwear and modification of activities that cause repetitive pressure on the foot.